What Nova Scotia can learn from the pandemic about delivering equitable health care
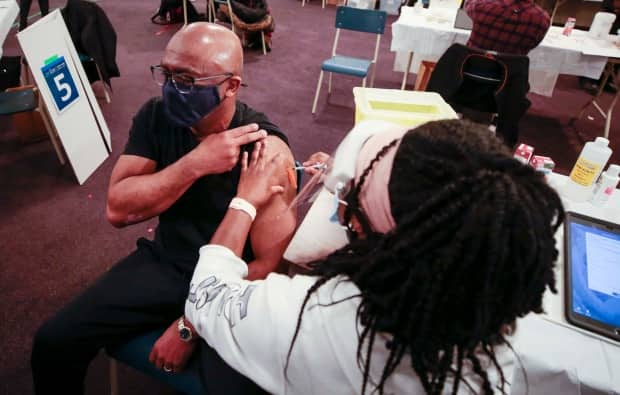
Several months into the pandemic, when vaccines were on the horizon, Sharon Davis-Murdoch and other leaders in the Black community started raising their voices.
"Having vaccine clinics generically would not address the needs of our people."
That was the message Davis-Murdoch, the co-president and a founding member of the Health Association of African Canadians, said she and others delivered to decision-makers in the Nova Scotia government late last year.
"We could anticipate that given the history and the lived reality of our people, there would be mistrust of this vaccine," she said.
The first culturally specific vaccine clinic opened in early April in the historically Black community of Upper Hammonds Plains.

By the end of July, Davis-Murdoch said there had been more than 2,000 people vaccinated at clinics in historically Black communities across the province, and some sites continue to operate. In her books, it's been a success.
What's more, the clinics could now serve as a template for the delivery of other health services in a way that addresses and ultimately aims to eliminate racial inequities, Davis-Murdoch said.
"We're not looking forward, and we sure hope there's not a second pandemic," she said. "But the fact is there will be other policy needs."
The vaccine clinics were put together quickly to respond to a pressing need, but before other health-care projects are planned through the lens of racial equity, existing inequities need to be better understood. They need to be made measurable.
To that end, Nova Scotia's Liberal government announced earlier this year it would begin collecting race-based health data.
Davis-Murdoch is a member of a working group for the fledgling initiative, along with representatives from the Iranian Cultural Society, the Bangladesh Community Association, the Immigrant Migrant Women's Association of Halifax and others.
Information Davis-Murdoch said she'll be looking to glean from the data includes the health status of Black Nova Scotians and their use of the health-care system across primary, tertiary and long-term care.
What's to come after the election
Although started by the Liberals, the race-based data initiative is likely to continue no matter which party forms government on Aug. 17.
The program appears in the NDP platform and leader Gary Burrill said recently on the campaign trail that it would be a priority for an NDP government.
The Progressive Conservatives do not specifically address health inequities in their platform, but leader Tim Houston said it would be wrong to say the issue is excluded.
"We're just very, very focused on health care, and that's for all Nova Scotians," Houston told reporters at an event last week.
"We recognize that it's more difficult for some than others and we want to make sure that we level that and that everyone has equal opportunity to the health care and mental health care they need in this province."
Davis-Murdoch said she was pleased to see the issue addressed in some platforms and leaders' remarks, but she'd hoped for more. She said she'd "continue to listen closely to what leaders and candidates are saying."
Davis-Murdoch said she expects community consultation on the data program to begin this fall, which will inform decisions about how to collect and use the information.

Meanwhile, Annie Morrison said she and her colleagues in the provincial health authority's public health division are starting to brainstorm about how to apply other lessons about health equity to life after the pandemic.
Morrison is a consultant with Nova Scotia Health's mobile unit, which was born last year to provide testing in outbreak zones around the province. There are now 10 vans that are deployed to communities across the province, as well as to shelters, long-term care facilities and jails to provide testing and vaccinations.
Morrison said the program is an acknowledgement that the risk of contracting COVID-19 can vary based on factors including race, gender, age and income.
What will come of the mobile units after the pandemic is still to be determined, Morrison said, but she said the approach has proven to be an effective way to overcome barriers to health-care delivery.

Post-pandemic, Morrison said the question will be what other barriers the mobile units could help to overcome. It's a question that she said she expects the health authority will try to answer in collaboration with community organizations, Black Nova Scotians, newcomers and people with disabilities.
"These are all folks that we know are underserved by our system currently. And we'd love to find ways that the mobile unit can help support that," she said.
When it comes to the Mi'kmaq, Morrison said it's often the case that health-care delivery is best left to the community.
"Sometimes we're not the best people to deliver services. [Sometimes] community can actually do it better. They have the relationships. They have the trust," she said.
"In these cases, it's more of us getting out of the way and providing supports that are available, but letting community deliver and do it the way they know as best."
Daphne Hutt-MacLeod echoed that. She's the director of mental health services at the Eskasoni Health Centre. She said mental health care that combines Western medical practices and Mi'kmaw cultural practices has proven to be the most effective approach.
The crux of the matter is that demand for mental health care in Mi'kmaw communities has recently surged, and Hutt-MacLeod said her clinic is struggling to keep up.
"With recent events, with the discovery of residential school survivor children's bodies, the demand has far outpaced the resources that we have."

Hutt-MacLeod said people are looking for family-based and community-based treatments.
"They want to be able to go somewhere where they can meet as an entire family, multiple generations ... so that people can understand why their grandparents were the way that they were or acted the way they did, because they may have been involved with the residential school system," she said.
Hutt-MacLeod said funding to pay for health-care services in Eskasoni is a patchwork of federal and provincial grants. She said her "dream" is to have sustainable funding to ensure consistent availability of mental health services.
MORE TOP STORIES

