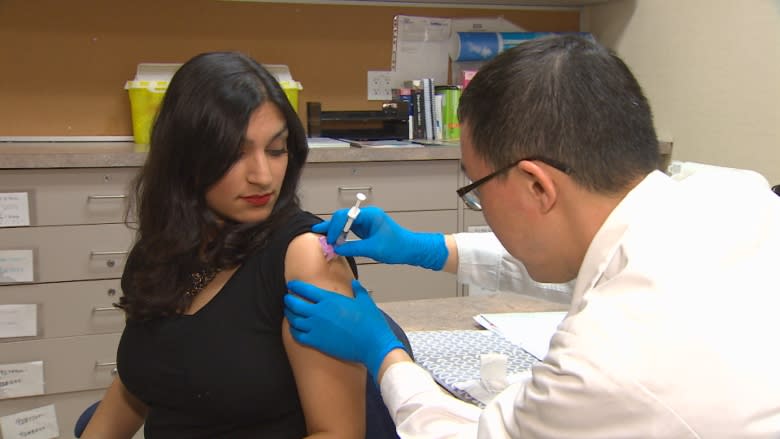
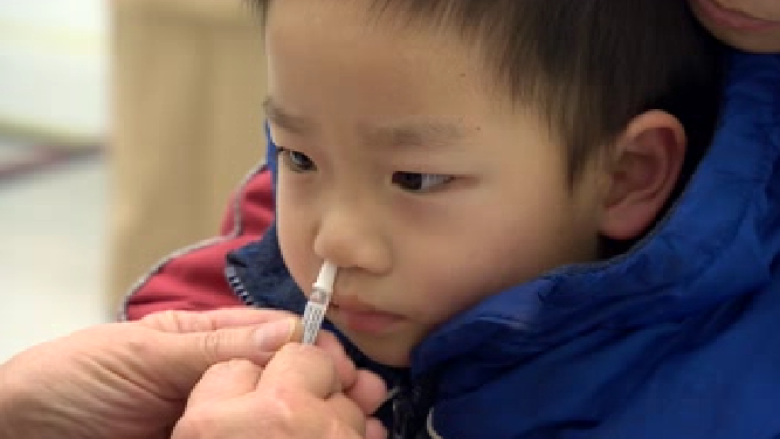
Why do Canadians avoid the flu shot?
News that H1N1 was the predominant strain of influenza this winter still wasn’t enough to convince Francisco Gonzalez to consider a flu shot.
In fact, he has never had one and says he is not convinced of the shot’s usefulness, in any case. “I just find most people are over-drugged, in general,” he said, adding that if he can’t pronounce something, it’s not going in his body.
To Gonzalez, 29, it does not matter if H1N1 affects more adults under 65 than other strains circulating in previous years. The flu is the flu, he said, regardless of its name.
Of course, Gonzalez is just one of millions of Canadians who don’t bother with flu vaccinations. Despite annual public-health campaigns about the importance of immunization, only somewhere between one-third and one-quarter of Canadians receive the shot each year, according to Statistics Canada data. What’s with the disconnect?
As Dr. Monica Hau puts it, there’s a discrepancy between the perceived risk of getting the flu and possible outcomes.
“People, I think, often don’t think they’re at risk or they’ll wait until they start hearing of reports of lots of flu cases, hospitalizations and death,” said Hau, the associate medical officer of health for Toronto Public Health. “And then, that might prompt them to get the flu shot. But it might be too late at that time because it does take two weeks for the flu shot to work.”
It’s easy to forget the risks of influenza, with the world being nearly a century removed from the Spanish influenza epidemic after the First World War. The 1918-19 outbreak killed about 50,000 Canadians and caused social and economic upheaval; the Canadian Encyclopedia notes that the federal Department of Health was launched in 1919 in response to the epidemic.
Nowadays, we’re in better health and enjoy the benefits of medical progress – not to mention becoming better educated in making healthy choices. Younger adults and people raising kids, for instance, were more likely to start getting flu shots, even if they didn’t bother in the past five years, found a Harris-Decima poll done for The Canadian Press. Still, flu shot rates remain stubbornly low. According to the poll, 39 per cent of respondents had not received a shot over the past five years and had no plans to get one this year.
Family doctor Jeff Kwong, who is also a scientist at the Institute for Clinical Evaluative Sciences and Public Health Ontario, puts immunization rates at somewhere between 25 and 40 per cent, depending on the year and the location. He has come across some reasons why people avoid flu shots – and most of them aren’t particularly persuasive.
First off, people think flu isn’t reason to worry, so a flu shot would be unnecessary, Kwong said in an e-mail. Otherwise, people don’t believe the shot is effective, worry about side effects or falling ill after receiving it.
“The problem is that flu shots are designed to only prevent infection from influenza viruses. There are many other viruses that can cause similar symptoms as influenza that flu shots do not prevent,” Kwong said.
Kwong added that the shot is about 60 per cent effective in preventing the flu, and said many studies show that most people opt to be immunized if their doctors recommend it. However, in many parts of Canada, with the exception of British Columbia, flu shots are not mandatory for health-care workers.
“Healthcare workers are seen as role models … But if doctors, nurses, and other healthcare workers are not getting vaccinated themselves, then it increases suspicion in the general public,” he said.
But a more common reason is something much simpler. According to Kwong, people just don’t get around to it.
People, I think, often don’t think they’re at risk or they’ll wait until they start hearing of reports of lots of flu cases, hospitalizations and death. But it might be too late at that time because it does take two weeks for the flu shot to work.
— Dr. Monica Hau, Toronto Public Health
This flu season, Alberta combined more publicity with better access to shots and saw a jump in vaccinations before the province ran out of vaccine. The shot was offered at more than 900 pharmacies, places where people could more easily park their cars and perhaps get a little shopping done.
“That gave us a lot more outlets, lot more reach within the province,” said Dr. James Talbot, chief medical officer of health at Alberta Health. He estimated the vaccination rate for this year at well above 26 per cent, making it the second-best year on record. In comparison, about 22 per cent of Albertans got the shot last year, while during the 2009 H1N1 scare, about 34 per cent were immunized.
“This was a year in which H1N1 came back and there’s brand recognition for H1N1 from the year that we were concerned it could cause a pandemic,” Talbot said.
Though Alberta is on track for a relatively normal flu season, a cluster of deaths early on, mostly in Calgary, may have also caused some local concern, Talbot said.
More analysis needs to be done to see what specifically made this year different, but Talbot said the changes made to Alberta’s flu-shot program were key.
“What we did this year was to open it up to see if we could encourage more people to come forward and get immunized. And that looks like it worked.”
Toronto’s Dr. Kwong had a different view about the run on flu vaccine in Western Canada. “It's human nature to respond to fear. Most people don't fear influenza most years (even though it kills thousands of Canadians – mostly elderly – every year),” he said. “But when people hear about young people being hospitalized or dying from influenza, they get scared and go get the vaccine.”
Really, though, the health professionals interviewed just want people to get the shot. “Some years it is more effective and other years it is less effective,” Kwong said. “But some protection is better than no protection.”