Pig kidneys successfully transplanted into human body for the first time

Two kidneys from a genetically modified pig have been transplanted into the body of a brain-dead human for the first time, in another groundbreaking cross-species operation.
The achievement has been described as a "game-changing moment in the history of medicine" and raises hopes of clinical trials in living humans with kidney failure in the near future.
Jim Parsons, 57, was a registered organ donor and dirt bike enthusiast who was in a serious accident in September 2021 that left him brain-dead.

While his organs were not viable for donation, his family consented for him to be part of a pioneering xenotransplant experiment to test the safety of animal organs in people.
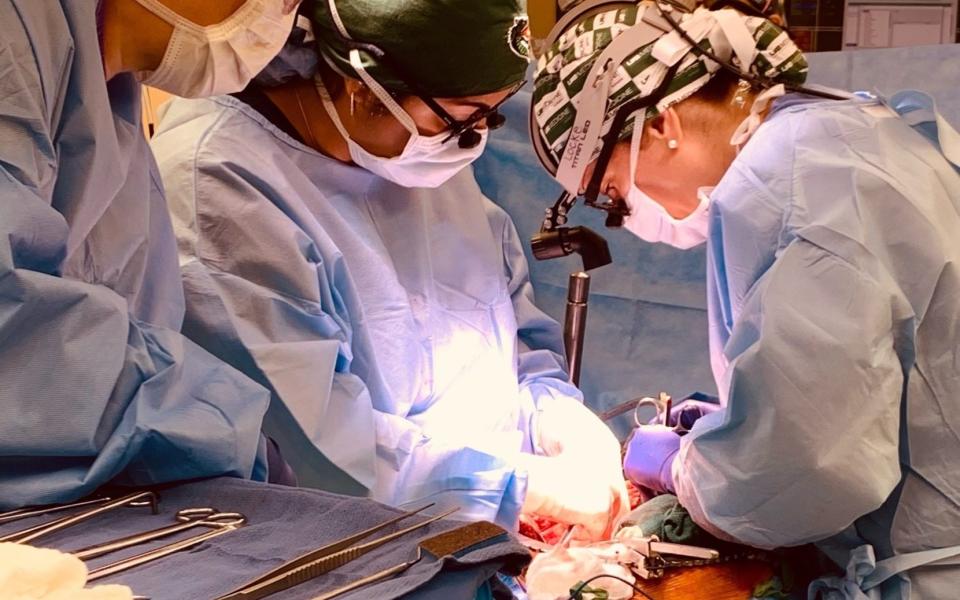
On September 30, doctors at the University of Alabama at Birmingham Hospital replaced Mr Parsons’s kidneys with two from a donor pig, a 13-month old boar weighing 350lbs.
The transplanted kidneys were able to filter blood, produce urine and, crucially, were not immediately rejected. The kidneys worked well for 77 hours until the experiment was terminated due to the failing condition of Mr Parsons’ body.
Scientists have been working on xenotransplantation - the use of organs or tissues from animals in humans - for decades and believe it is the most pragmatic solution to the organ shortage crisis that sees thousands of people a year die while waiting for transplants.
A company in Virginia called Revivicor - a spin-off company from PPL Therapeutics, which created Dolly the sheep, the world’s first cloned mammal - produced the pig, which had 10 genetic alterations designed to ensure its organs would be safe and effective.
Xenotransplants are getting increasingly closer to a clinical reality, and this study lays the groundwork for larger trials.
Last week, David Bennett from Maryland became the first living person to receive a successful animal organ when he was given a genetically modified pig heart.
But the study involving Mr Parsons is the first to ascertain that brain dead individuals work well as a preclinical human model, a crucial step forward in making xenotransplants a reality for the millions of people worldwide waiting for lifesaving organs.
“This game-changing moment in the history of medicine represents a paradigm shift and a major milestone in the field of xenotransplantation, which is arguably the best solution to the organ shortage crisis,” said senior author and the surgeon who performed the transplant, Dr Jayme Locke.

“The concept of being able to have an organ waiting on the shelf, waiting for the person who needs it, is just remarkable to think about, and exciting for that person.
“I feel really privileged to be just a tiny part of a really big puzzle that people have been working on for many years.”
One major question which has now been answered was whether pig organs could cope with the higher blood pressure in humans. The pig kidney coped just fine, the scientists report in their study, published in the American Journal of Transplantation.
As a result of this vital advancement in the field, Dr Locke has named the experiment, which will likely be used in future as a blueprint to ensure animal organs are safe for people, “The Parsons Model”.
Ms Julie O’Hara, the ex-wife and friend of Mr Parsons, said: “I cried when [Dr Locke] told me about that proposal, to name this after Jim.”
“Jim would have wanted to save as many people as he could with his death, and if he knew he could potentially save thousands and thousands of people by doing this, he would have had no hesitation,” said Ms O’Hara.
“Our dream is that no other person dies waiting for a kidney, and we know that Jim is very proud that his death could potentially bring so much hope to others.”
Still a 'long way' to go
Prof Gabriel Oniscu, president-elect of the European Society of Organ Transplantation and director of the Edinburgh Transplant Centre, told The Telegraph: “This is another landmark study on a number of levels.
“All of a sudden, we've created potentially a new way of testing [xenotransplant] therapies prior to going to clinical trials.”
He added that the experiment was “great progress” but still experimental and we are a long way from xenotransplants becoming a reality.
“Xenotransplants will not be an option for everyone, but they may become an additional option. Until that happens and we know that it's safe, we still need to rely on donations.”


