As workloads increase in Sask. ICUs, health-care workers are considering other careers: union president
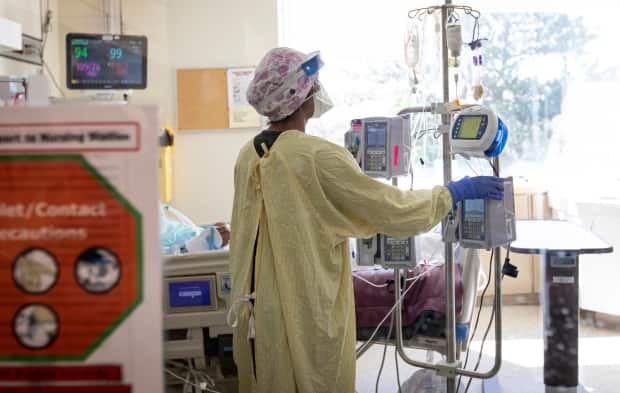
As Saskatchewan approaches the 15th month of the COVID-19 pandemic, health-care workers are continuing to deal with the effects of a health-care event that has worsened with time.
Industry heads say workers are openly considering their futures in the field after more than 14 months on the front-lines.
"It's happening now. It's happening right now as we speak," said Tracy Zambory, president of the Saskatchewan Union of Nurses (SUN).

Zambory said in an interview Friday that union members have told her that they just can't take the stress and anxiety anymore and are burning out.
Others are ready to pack it in altogether.
As cases of the virus have spiked in 2021 and the demographics of those appearing in intensive care units (ICU) have shifted younger, the effects have become even more pronounced, said Zambory.
"There is no words to describe what it's like to hold an iPad up so family can say goodbye to their loved one," she said.
"When those families are getting younger and younger, when it's little kids who are saying goodbye to their parent, it is taking a toll."
The complaints of long hours and few breaks aren't just anecdotal.
According to information released during a weekly doctors' town hall, there's now data showing the change in workload in the province's ICUs.
During the first quarter of 2021, there was a 192.5 per cent increase in the number of hours worked when compared to the same time last year.
That's the equivalent of an additional 260 full time employees.
Despite the increase, only been 74 employees have been added to offset the workload.
"We're going to have to work with a lot of front-line health-care workers on how they've managed their way through this pandemic and we're going to be have to be there for them in a whole lot of ways once we find our way through this," said Zambory.
The province did not answer a request for response to the figures on the increase in ICU hours as of the time of publication.
Although the ICU in Regina is already facing issues with capacity, the information released by the SHA indicates Saskatoon is approaching increased occupancy.
Urban areas are not expected to return to baseline capacity for some time, according to the presentation.
Zambory said that the hours and stress are like nothing her organization's members have ever seen.
"In our intensive care units, it's constant. And this was not the norm prior to the to the pandemic," she said.
She said SUN has committed to working with the government to find solutions. That includes a push to strengthen the province's mental health strategy to avoid and treat burnout.
Zambory said she is cautiously optimistic about Saskatchewan's vaccination strategy providing a way out of the continued pandemic, but that the province needs to pay attention and do what's necessary if cases spike or hospitalizations increase.
"It comes down to what can we do to help? And part of that is to take the vaccine that's offered to you. It's the best one. Follow the public health orders so that we can take that pressure off the health care system," she said.

