With hospitals overwhelmed, can Canada overhaul health care for the long term?
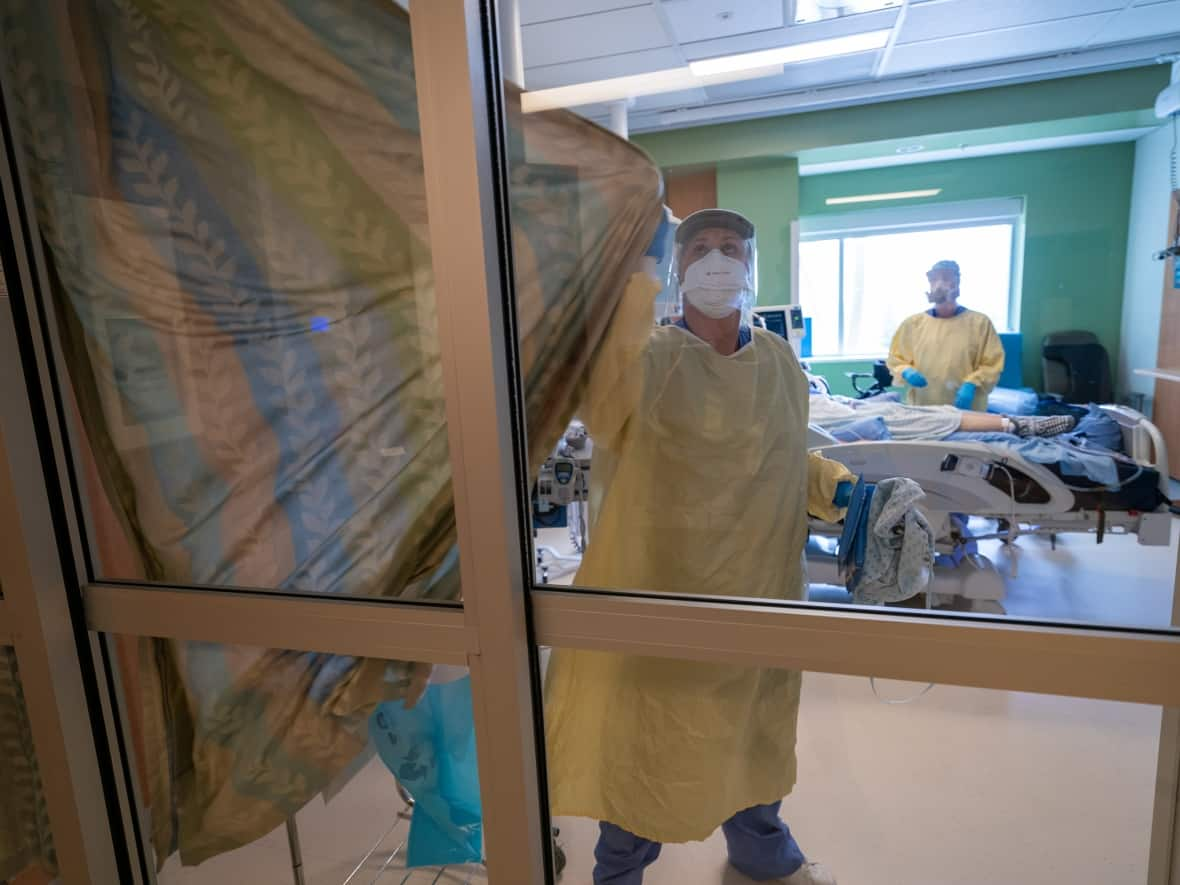
As hospitals strain under the burden of record-high numbers of COVID-19 patients, two former health ministers warn that there is no silver bullet that can reform the health-care system and safeguard it for the long run.
"People always want to have a quick single solution to a complex problem," former federal health minister Jane Philpott said in a panel interview on CBC's The House, which aired Saturday. "There is not a single thing that will fix the whole picture."
"Spending more money to do a lot of things the same way that we've always done them" will not fix structural issues with resource allocation and the workforce, added Fred Horne, a former Alberta health minister.
The stresses of COVID-19 hospitalizations, driven by the current wave of infections, are being felt acutely across the country, including in Quebec.
In Montreal, ER nurse Marie-Pier says she worries that cratering morale could lead to a collapse in the hospital system. CBC News is using only her first name because she fears disciplinary action for speaking out.
"My biggest concern is that I am mostly scared that we're just going to crumble and literally have nurses stop working, people stop working period, or completely change profession because it's too much," she told host Chris Hall.
She said health-care workers are exhausted, and while many try to keep working and push through, sometimes they simply burn out because of stress and fatigue after several waves of the pandemic.
"Out of nowhere, we just fall."
Marie-Pier said steps such as increasing pay, reducing forced overtime and creating better overall conditions would help to bring workers back into the health-care system.
"It's a beautiful job. I love to care for people just to help people to feel better and to be able to see them rise and leave the hospital after," she said.
Hospitals under stress across country
Similar workforce and resource strains are being felt across the country, prompting questions once more on how the health-care system, which experts say can be overwhelmed during a normal flu season, can be reinforced and reformed for the long term.
"Most Canadians would agree that even before COVID-19, our capacity was often stretched too thin," federal Health Minister Jean-Yves Duclos said earlier this month.
A key question in the debate over a potential solution is the role of the federal government. Over the past two years, provinces have consistently asked for Ottawa to boost its health-care transfer to provinces — up to 35 per cent of costs versus the current 22 per cent.

Prime Minister Justin Trudeau has said he is open to renegotiating the transfer system once the pandemic is over.
"I think that it's a good time for the federal government to exert itself more strongly in the health space, and we do need more investments," said Philpott, who served as federal health minister from 2015 to 2017.
But she cautioned that there is a need for other reform as well, because "you can't keep throwing more money at doing things the same way we've always done.
"People know how much care is needed in hospitals, but we also need to spend in places like home care and mental health and primary care," she added.

Changes to support the workforce, such as allowing easier movement of workers from province to province and more efficient assignments of physicians versus nurses or general practitioners, would also help, Philpott said.
"There are very few provinces that have a really good workforce plan, and there is no existence of a national health workforce plan. So that would be an area that I would put a lot of attention to if I were a federal minister."
Horne, who served as provincial health minister in Alberta from 2011 to 2014, said transformational change of the type that's needed "takes a lot longer than one political cycle or one budget cycle."
Privatization debate a 'red herring,' Philpott says
Both former ministers expressed skepticism that the debate over private health care was a fruitful one.
"I think the whole issue of public-private [care] is highly misunderstood and can often be used as a red herring," Philpott said. There is a great deal of private delivery already built into the system, she said, and the concern should be making sure privately paid systems don't disrupt access to care for all.

Horne said that during his time in office, private delivery of publicly insured services had not been a "huge issue" in his conversations.
"In fact, [people] were expecting us to make best use of the public funds — and that includes, you know, partnerships with the private sector and industry as appropriate," he said.
Philpott said that "we're actually starting to see some good things happening behind the scenes," such as a national data health plan, but to push forward requires strong collaboration between levels of government.
Horne said his advice to health ministers now is to focus on accomplishing things that will survive their tenure as head of the system.
"It's a tough grind," he said.


