Mom transports severely ill daughter in own vehicle after ambulance transfer delays
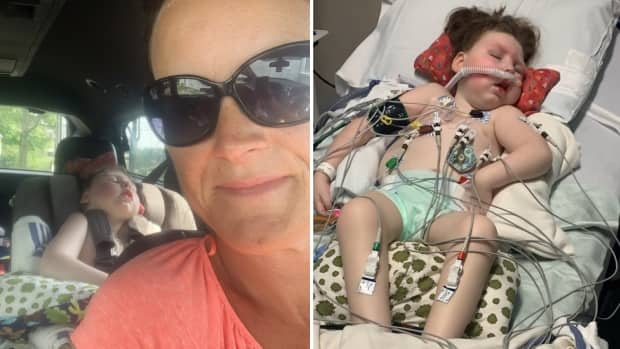
A Nova Scotia mother is raising questions about wait times for ambulance patient transfers after sitting at the hospital for seven hours before giving up and driving her seriously ill daughter in her own vehicle.
"It's the letdown and disappointment. I had my whole room packed, I was ready to go," said Kristen Langille, whose eight-year-old daughter Georgia was receiving treatment at the IWK hospital in Halifax.
They had been there since Sunday after Georgia, who has a rare disorder, was taken to hospital with pneumonia. Georgia is blind and deaf, has no muscle tone and suffers from repeated seizures due her condition of congenital disorder of glycosylation Type 1P.
She had been airlifted to the IWK from Truro, N.S., where the family lives, and was waiting Tuesday to return to the Colchester East Hants Health Centre in Truro, about an hour's drive from Halifax.
Langille said the nurse on her daughter's unit had booked the ambulance patient transfer at first for 9 a.m. that day. Transfers typically happen when patients are being taken from one medical facility to another.
"They came back and said now it's going to be 1 p.m., then they said 3 p.m., then they came back and said 4 p.m., and then they said there is no ETA, it's going to be hours," Langille said. "I had a couple of cries, and I usually don't cry, and I just was feeling defeated."
Pandemic pressures create additional challenges
After several days away from home and knowing a bed was waiting at the Truro hospital, Langille then decided to take Georgia in her own van, even though she was still hooked up to two intravenous lines and normally her mother would not even drive her across town.
They made it there safely, but Langille is now calling for action on ambulance patient transfers and said she will be writing to her MLA.
She's seen repeated delays after needing at least 40 transfers throughout her daughter's life, which has involved frequent hospital care.

Emergency Health Services, which operates the province's ambulance system, acknowledges the volume of patient transfers has been increasing as Nova Scotia comes out of the third wave of the COVID-19 pandemic.
That has led to additional pressures, as the system catches up with patients returning to elective surgeries that were postponed during the lockdown.
"There is our transfer volume that would normally exist and then above and beyond that we have these additional bookings that are coming in," said Charbel Daniel, the executive director of provincial operations with EHS. "I understand the frustration and our goal is always to make sure people are moved in a timely fashion."
Daniel, who cannot speak to Langille's specific case, said EHS is doing what it can to adjust to the situation. Among a number of measures, it has hired 55 new paramedics since the start of the year, but is experiencing unique challenges he attributes to the pandemic.
"We are navigating a fatigued workforce that has just been through a pandemic and we're ensuring they have the appropriate time off to rest and regenerate," he said, adding support programs are also being offered to staff.
'It's not the fault of paramedics'
Daniel maintains ambulance patient transfers are still able to meet the demand while stressing unpredictable situations are always possible.
"We have to factor in that if a large number of emergency calls come in at that same time, and given our deployment system that could affect those times and they may have to be rebooked," he said.
A new patient transfer model is being piloted in the west and central zones of the province. It involves a van in each area that can transport six or seven patients at a time as a way of easing stress on the system.
The union representing paramedics sees what happened to the Langille family as another sign of a bigger issue in emergency medical care.
"We are at a breaking point here and it's not the fault of the paramedics," said Michael Nickerson, the business manager for the Nova Scotia Paramedics International Union of Operating Engineers Local 727. "I feel for that lady and her daughter. It's terrible and that's just one example."

Nickerson said many of his members are "burned out" from long overtime hours and doesn't believe it can be put down to the response to COVID-19.
"This was happening before COVID, their 12-hour shifts often become 14- or 15-hour shifts and they need a work-life balance and they're not getting that right now," Nickerson said.
Due to privacy reasons he could not say how many paramedics are currently taking time off, but said more mental health supports are needed in addition to a more manageable workload.

