N.B. woman spent 20 years in pain, now she's ready to get her life back


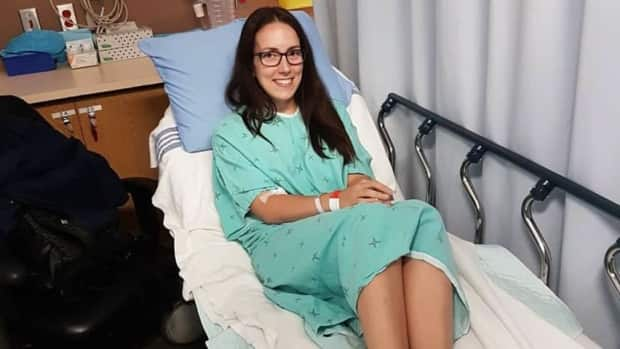
For more than 20 years, Nicola Sleep has endured excruciating pain for up to two weeks of every month.
It feels "like razor blades in my stomach, or if someone poured acid in your abdomen and just left it there," she says.
Her only escape has been to "live in" a hot bath or to curl up in the fetal position with a heating pad until it numbs, or sometimes even burns, her skin.
Sleep, 32, of Upper Gagetown, suffers from severe endometriosis, which flares up during menstruation and ovulation.
Endometriosis occurs when cells similar to the lining of the uterus implant abnormally outside the uterus and form lesions, cysts and other growths.
The disease affects about one in 10 girls and women, and an unknown number of transgender, non-binary and gender-diverse people, according to Endometriosis Network Canada.
In Sleep's case, it's "attacking" her bowel, bladder and kidneys and causing fertility problems. But this summer, she will undergo a surgery she hopes will change her life.
Dr. Craig Morton will perform laparoscopic gynecologic surgery to identify and remove the tissue that has grown abnormally and "unstick" her organs that have fused together.
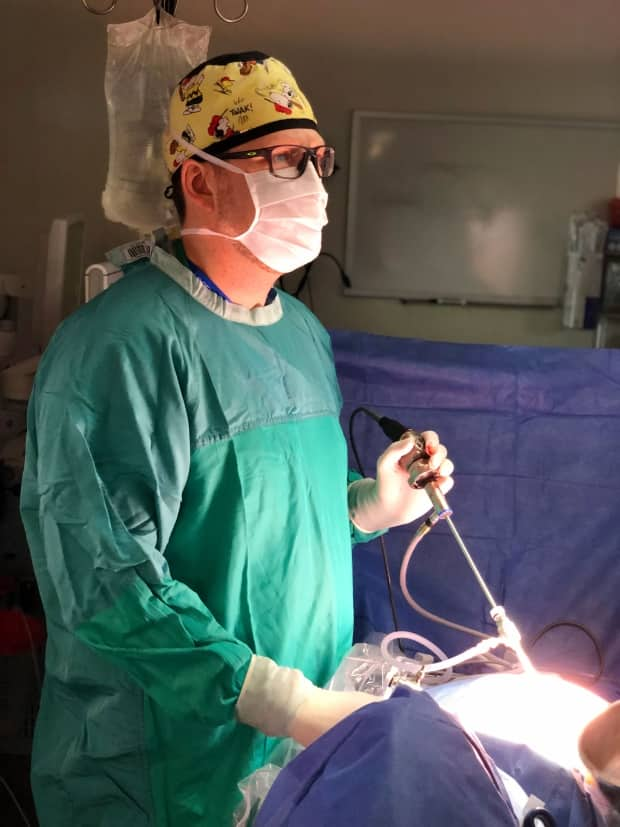
Morton, her Saint John-based gynecologist, left his practice nearly a year ago to complete a surgical fellowship in Calgary in this specialized endometriosis care.
There is no known cure for endometriosis, but he says excision surgery has become the gold standard.
Laparoscopic surgery is when surgeons use small incisions to insert a laparascope, a thin, flexible tube with a light and a small video camera on the end, along with other instruments, and operate while viewing detailed images instead of opening the patient up.
Excision surgery involves removing the entire endometriosis lesion, whereas ablation surgery treats only the surface of the lesions, which may go deeper and could grow back.
Morton feels there is "a void" in New Brunswick when it comes to caring for people with endometriosis.
"I found myself wanting to be able to do more for patients, both surgically and medically, and there really wasn't a lot of other providers around."
He was often forced to send his patients to Nova Scotia, Ontario and Quebec. Even then, they faced "significant" delays to be seen and treated, often more than a year, he said.
"So that's really what prompted me to want to further my skills and training, to be able to offer care, but also to be able to support colleagues who were also struggling with, you know, being able to care for complex patients."
'Suck it up'
Sleep can barely contain her excitement about her surgery, tentatively set for July. After years of searching for answers and fighting for her pain to be taken seriously, Morton is a "light in the darkness of endometrosis" for New Brunswickers like her.
Sleep's journey began when she was about 10 years old, shortly after her period started.
Most days, she was just "a regular kid," going to school and playing sports, such as hockey and soccer. Then during her period week, "it would be like instantly, I'm a whole different person, crying and [in] pain."
And trying to explain to her coaches why she wasn't performing to the top of her ability, or why she was doubled over before a game or practice wasn't any easier. "They're like, 'OK, well suck it up, every girl has cramps.'"

By the time she was 12, she was put on birth control pills to try to alleviate the unbearable pain and heavy bleeding.
When she hit her 20s, she started to do her own research. "I said, 'This isn't normal, I need help.'" That's when she discovered endometriosis and took the information to her "amazing" family doctor.
Sleep was diagnosed with suspected endometriosis but continued to suffer in pain.
Perhaps the most difficult thing about this condition has been her fertility struggles.
'It's not just in my head'
"My whole life I've dreamt to be a mom. And then when I thought I couldn't, it was heartbreaking," said Sleep.
Her family doctor referred her to Morton, who was relatively new to his practice at the time. He sent Sleep and her husband Chris to a fertility clinic for in vitro fertilization, where mature eggs are retrieved from the ovaries and fertilized by sperm in a lab and then the fertilized egg, or embryo, is transferred to the uterus.
To prepare, Sleep had a laparoscopic surgery, which confirmed she had Stage 4 endometriosis with endometriomas, or cysts inside the ovaries, which had to be removed.
She felt validated when she saw the video images. "I felt like, 'You know what? All that pain, there's a reason. It's not just in my head,'" she said.
When she saw how "messy" her insides were, she felt like being her own advocate had finally paid off.

The in vitro didn't work, but she did eventually get pregnant. "I was over the moon," said Sleep.
Their "miracle" son Jack was born about 10 weeks premature and spent about 60 days in hospital, but is "a fighter" and now 20 months old.
She wants to give Jack a baby brother or sister but has been unable to conceive and is in too much pain to keep trying.
In frustration, she went to Morton about a year ago, saying, "Cut it out of me. Take everything out. Take my uterus, take everything."
But he told her he was about to start his fellowship and encouraged her to hold off.
"I'm so excited because now he has a full year of endometriosis knowledge and he's ready to try to help me get my life back," she said.
Up to 9 years for diagnosis common
Sleep's experience is typical, according to Morton. On average, women wait between seven and nine years from the onset of symptoms just to get a diagnosis, he said.
Access to specialized care can take another year or two, and if they decide on surgery, they usually wait another six to 18 months, depending on the urgency of their situation.
One of the main reasons it takes women so long to get diagnosed, said Morton, is the "societal normalization of painful periods — this notion that periods should be painful."

Another factor is what he describes as historically insufficient health-care provider education and awareness about endometriosis. "A lot of providers don't have the tools to be able to confidently diagnose endometriosis."
Specialized training hasn't existed for very long either, he said.
That is slowly changing though, said Morton.
He expects to be busy when he returns to Saint John at the beginning of May, provided he can secure the necessary operating room time.
Sleep is one of numerous patients still on his wait list, he said. He also anticipates a "significant increase" in referrals.
Not alone
Being able to help women with this "common, chronic and sometimes debilitating condition" is "very near and dear to [his] heart," he said.
"A lot of women have really felt like their symptoms have either been dismissed or not heard by their health-care providers and sort of pushed aside as either normal or, you know, dramatic."
The majority of them are of reproductive age, but pain prevents them from being able to engage in activities for weeks at a time and strains their relationships, he said.

Morton hopes to eventually see New Brunswick offer an interdisciplinary clinic for the management of endometriosis and chronic pelvic pain, like the one in Halifax, which opened in September 2021, the first of its kind in Atlantic Canada.
Sleep is encouraged that more people are becoming aware of endometriosis and now have access to trained professionals and support.
She urges anyone with unusual pain to "keep fighting" to be heard.
"You're not alone," she said. "You don't have to suffer alone."


